Central lymphatic surgery
Abstract
In recent years, microsurgical reconstruction of the lymphatic system has opened new frontiers in the treatment of central lymphatic lesions. Central lymphatic lesions can be congenital or acquired. While the latter can result from any surgery or trauma in the area of the thoracic duct, congenital lymphatic lesions can show a plethora of manifestations, ranging from singular thoracic duct abnormalities to complex multifocal malformations. Regardless of the anatomical location of the thoracic duct lesion, these conditions cause recurrent chylous effusions and downstream lymphatic congestion and are associated with increased mortality due to the permanent loss of protein and fluid. In case of disruption of the lymphatic flow, microsurgical reconstructive surgery is indicated to treat downstream congestion leading to bronchitis plastica, protein-loosing enteropathy, chylothorax, and chylascites. Thoracic duct-vein anastomoses can reconstruct the physiological lymphatic flow.
Keywords
INTRODUCTION
Central lymphatic lesions may arise in the course of trauma and surgery or be congenital. The latter are classified as primary lymphatic anomalies, which can show very different manifestations, ranging from singular thoracic duct lesions to complex multifocal malformations. The overall prevalence of primary lymphatic anomalies, including lymphatic malformations as well as primary lymphoedema, is 1:4,000 live births, with some patients not developing symptoms until adulthood[1,2].
Thoracic duct injuries typically occur in the setting of head and neck surgery such as neck dissection, pharyngectomy, esophagectomy or thyroidectomy or after heart surgery. After lateral neck dissection, the incidence is 4.5-8.3%, with the risk increasing with the presence of metastases at the angulus venosus as well as the extent of surgery[3-8]. Depending on the anatomic location involved, patients suffer from leakage of chyle in the area of the surgical wound, recurrent thoracic (chylothorax) or abdominal chylous effusions (chylous ascites), which favor infections and further complications due to permanent protein and fluid loss leading to a mortality of up to 50%[9-10].
Lesions of the central lymphatic system or lymphatic dysfunction due to high venous pressure can also result from Fontan surgery in patients with congenital heart disease with single-ventricle physiology. In these patients, lymphatic dysfunction can lead to hepatic lymphatic congestion, protein-losing enteropathy and plastic bronchitis due to the formation of rubbery and caulk-like plugs in the airways, causing severe respiratory issues. Protein-losing enteropathy is caused by permanent enteric protein loss, resulting in hypoalbuminemia, lymphopenia, hypogammaglobulinemia, and loss of clotting factors[11].
Congenital malformations of the lymphatic system include central conducting lymphatic anomalies (CCLA) and lymphocele.
Due to the rarity of central lymphatic lesions, diagnosis and treatment should be reserved for specialized lymphatic centers. In addition to a detailed history, diagnosis is based on special imaging, preferably magnetic resonance lymphangiography (MRL), which allows accurate visualization of the central lymphatic lesion and is essential for precise treatment planning[12]. In the case of lymphatic lesions in childhood, a broad genetic workup should also be performed[1].
TREATMENT ALGORITHM
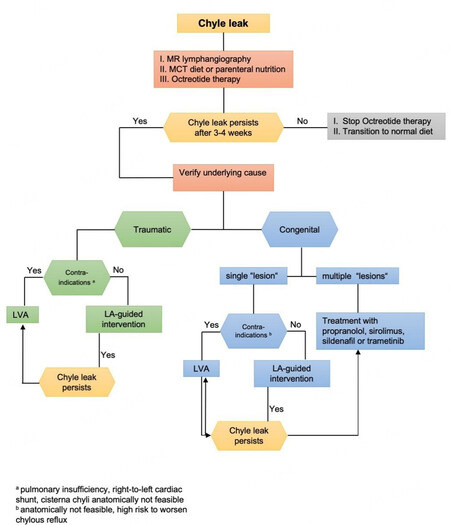
We previously established a treatment algorithm based on a series of cases with central lymphatic lesions, which is shown in [Figure 1]. Initial treatment of central lymphatic lesions should be based on conservative therapy including a diet of medium-chain triglycerides (MCT) or total parenteral nutrition (TPN). Although success rates vary widely, this therapy can lead to spontaneous resolution of the chyle leak[13,14]. In addition, we propose to combine dietary measures with an Octreotide therapy that is supposed to reduce the production of chyle. Especially in patients with central conducting lymphatic anomaly (CCLA), other substances such as propanolol, sirolimus, sildenafil or trametinib are increasingly used[15-18].
Figure 1. Treatment algorithm for central lymphatic lesions[35].
When conservative treatment fails, lymphangiography-guided interventions remain the treatment of choice for central lymphatic lesions and allow for different treatment modalities depending on the entity of the lesion. Lymphangiography alone has been shown to succeed in different sites of lymphatic leakage due to its known Lipiodol-induced selective blockage of pathological lymph ducts.
Lymphangiography-guided embolization of the affected central lymphatics by endovascular coils or liquid embolic agents has been shown to be effective in postoperative chylous fistula, chylothorax, and chylous ascites with cure rates of 80-90% and overall complication rate of 7%[19,22]. However, it has to be considered that occlusion of the thoracic duct carries the risk of protein-losing enteropathy, lower extremity lymphedema, or worsening of lymphatic reflux with a fistula at another site due to the resulting down-stream congestion[23]. The same accounts for the surgical ligation of the thoracic duct, which has also been performed to treat patients with chyle leaks in the past[8,24]. In recent years, micro- and super-microsurgical reconstruction, defined as microsurgery in less than 0.8 mm vessels[25], has opened new frontiers to successfully treat rare central lymphatic lesions by thoracic duct-vein anastomoses.
ACQUIRED CENTRAL LYMPHATIC LESIONS
Traumatic interruption of the thoracic duct, either by trauma or more often through surgery within the neck and mediastinum (e.g. resection of neck and esophageal tumors, heart and aortic surgery, etc.), usually leads to persistent chyle leaks into wound or body cavities. Often these leaks are not reactive to conservative therapy alone. Due to the embryology of the central lymphatic system, disruption of lymphatic flow at the site of the lesion will, in most cases, not lead to downstream congestion, because dual ducts and spontaneous lympho-venous anastomoses are often present. Therefore, interventional embolization of traumatic chyle leaks is usually performed as a first-line therapy [Figure 1]. However, if a cutaneous chyle fistula drains via an open wound, reconstructive surgery can be considered during wound revision. In addition, interventional treatment may not be possible due to the absence of the cisterna chyli. In recent years an increasing number of reports have demonstrated that central lymphatic lesions causing severe chylothorax and chylous ascites can be successfully treated by thoracic duct-vein anastomosis in the retroperitoneal area and at the neck, depending on the location of the chyle leak[24,26-30]. Alternatively, chylous ascites can be treated by a deep inferior epigastric-based lymphatic cable flap connected to a gastroepiploic lymphnode flap. The latter may offer a new approach for patients with severe refractory chylous ascites[31].
Previously, we treated a 52-year-old patient with a thoracic duct fistula after left modified radical neck dissection for hypopharyngeal carcinoma and lymphogenic metastasis. The patient had also received neoadjuvant radio-chemotherapy. The diagnosis of thoracic duct injury was made on the basis of a postoperative milky drainage secretion of 50-170 ml/24 h and confirmed by the assessment of chylomicrons in the fluid and by conventional lymphangiography on postoperative day five. Conservative treatment based on a low-fat medium-chain triglyceride diet and an additional treatment with Octreotide was continued for five weeks but remained unsuccessful. A missing cisterna chyli, which would have allowed percutaneous access to the thoracic duct, led to the decision to perform microsurgical reconstruction of the thoracic duct. During surgical revision, parenteral administration of high-fat cream at the beginning of the surgery allowed rapid identification of the persistent chyle leak. Subsequently, an anastomosis between the external jugular vein and the thoracic duct was performed. The postoperative course was uneventful. Currently, the follow-up has reached five years, with no recurrence of chyle leakage[24].
CONGENITAL CENTRAL LYMPHATIC LESIONS
Surgical treatment of congenital central lymphatic lesions, such as central conducting lymphatic anomalies (CCLA), is much more complex because it usually affects the whole paraxial lymphatic system, which results in multiple areas of chyle leakage and may include insufficient lymphatic tonus and peristalsis[9]. The thoracic duct may be completely absent, resulting in lymphatic collateralization in the subcutaneous or muscular planes or leakage into the body cavities, such as pleura, pericardium or peritoneum. In addition, it may result in significant congestion of the lymphatic system of the liver and/or the gut entailing liver lymphorrhea and protein-losing enteropathy. Lower limb lymphedema and anasarca may additionally be present. Often insufficient collateralization of the interrupted central lymphatic flow is present necessitating reconstructive procedures of the central lymphatic system.
Only a few reports on central lymphatic surgery exist for these rare entities[32,33]. In a report about 14 patients, complete remission of symptoms was seen in five patients, and 50% of patients did not have any improvement. Of note, the majority of these patients showed a patent anastomosis with drainage of contrast agent in the venous system, confirmed by postoperative fluoroscopic contrast lymphangiography which emphasizes the complexity of the disease with an insufficient and discoordinated lymphatic peristalsis despite patent microsurgical anastomoses[33]. Kovach et al. performed thoracic duct-vein anastomosis in the neck in four patients with central lymphatic abnormalities of different etiology, achieving complete remission in three patients and partial resolution in one patient[34].
Thoracic duct-vein anastomoses can be performed on different levels depending on the localization of the lesion. In CCLA, often a lymphatic malformation can be found or severe congestion, e.g., in atresia of the thoracic duct junction at the left lympho-venous angle, may result in a dilated and tortuous thoracic duct. The best accessible region is the neck where usually low-pressure veins, e.g. the external jugular vein or paravertebral veins, are available. This is why most case series describe anastomoses in this region.
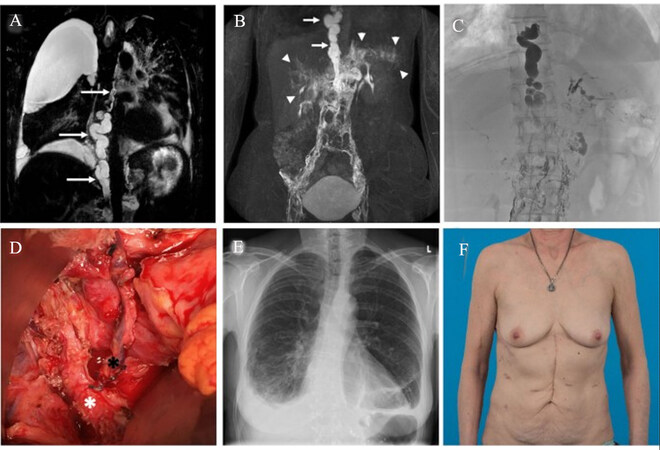
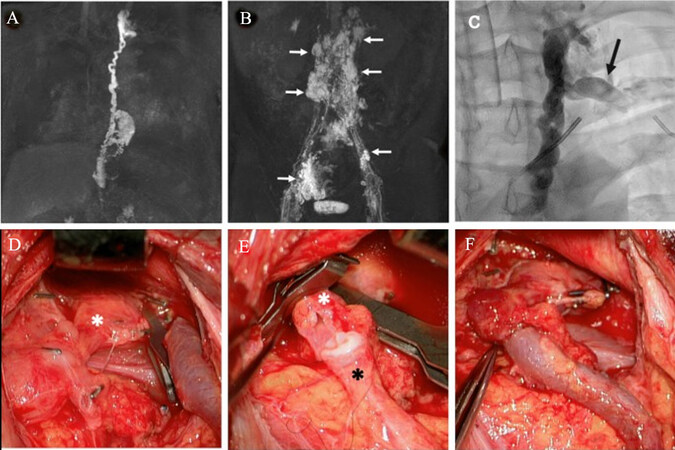
However, often in CCLA, thoracic duct abnormalities and interruptions occur at lower levels within the thorax or abdomen. This is why lympho-venous anastomoses of the thoracic duct should also be considered in these regions. We performed thoracic duct-vein anastomosis in a 52-year-old woman and a 34-year-old male with late onset of CCLA. Both patients were otherwise healthy but suffered from permanent chylothorax and chylous ascites in the setting of CCLA, with daily secretions of up to 3000 ml and recurrent infections due to immunodeficiency [Figures 2 and 3]. In both patients, stenosis of the thoracic duct with consecutive chylolymphatic reflux into the abdomen and thorax could be identified by MRL. While conservative treatment based on an initial MCT diet followed by total parenteral nutrition failed,lymphangiography-guided embolization of refluxive lymph vessels or even a thoracic duct embolization would have carried the risk of worsening chylolymphatic reflux and congestion.
Figure 2. MR-lymphangiography[35](A: non-contrast; B: contrast-enhanced) shows a massive dilatation of the TD and stenosis in the mediastinum (white arrows) with consecutive extensive chylolymphatic reflux into phrenic, pancreatic, and periportal lymphvessels (arrow heads). Observe also the bilateral pleural effusion (right > left); C: X-ray lymphangiography confirms dilatation and stenosis of the TD and reflux in the upper abdomen (a–c University Hospital Bonn, Department of Diagnostic and Interventional Radiology); D: The TD was ligated, and the caudal stump (white asterisk) was anastomosed end-to-end to the left phrenic vein (black asterisk); E: At 1-year follow-up, the patient is still asymptomatic with only marginal bilateral costophrenic angle effusion, and F: an inconspicuous abdominal scar.
Figure 3. A, B: Contrast-enhanced MR-lymphangiography demonstrated enlargement and tortuous configuration of the TD as well as reflux into retroperitoneal and pelvic distended/cystic lymphatics (white arrows); C: X-ray lymphangiography-guided catheter intervention showed a stenosis of the TD at the level of the angulus venosus sinister. Cannulation of the terminal TD (black arrow) was unsuccessful due to an extensively torqued TD so that a recanalization attempt was without success (A–C University Hospital Bonn, Department of Diagnostic and Interventional Radiology). D-F: The TD (white asterisk) was anastomosed end-to-end to the left external jugular vein (black asterisk)[35].
Thus, we performed a microsurgical anastomosis of the thoracic duct to a nearby vein to restore lymphatic drainage. In one patient, the lympho-venous anastomosis was performed for the first time subdiaphragmal to a phrenic vein resulting in complete resolution of the therapy-refractory chylothorax. In this patient, abdominal and thoracic drains could be removed by days eight and fourteen, given an output below 10 ml/24 h. At a two-year follow-up, this patient is still asymptomatic.
In the other patient, the thoracic duct was anastomosed to the left external jugular vein. Although anastomosis was patent and output from the abdominal drain decreased significantly, only partial remission could be achieved[35]. In this patient, the thoracic duct at the neck and within the thorax was severely dilated, indicating a lack of tonus and peristalsis. Whether this was due to the long-time chronic pressure at the occluded left venous angle or due to a congenital hypomotility of the thoracic duct could not clearly be distinguished. This, however, underscores the importance of early reconstructive treatment and the relevance of a toned thoracic duct in order to transport the chyle against gravity.
In our experience, venous pressure in the selected vein for lymphatic anastomosis should be low to facilitate lymphatic flow from the thoracic duct into the venous system. Alternatively, if higher venous pressure exists, a vein graft with valves can be interposed because, under physiologic conditions, a valve is present at the left lympho-venous angle preventing the reflux of venous blood into the thoracic duct. Furthermore, when performing thoracic duct-venous anastomoses in the abdomen, veins connected to the caval system should be chosen, as there is no experience to date on the effects of additional chyle flow into the portal system.
FUTURE PERSPECTIVES
We have recently demonstrated the feasibility and safety of the Symani Surgical System (Medical Microinstruments (MMI), Wilmington, USA) for lymphatic microsurgical procedures[36,37]. The Symani Surgical System, which has been solely developed for robotic microsurgery, provides several valuable features such as motion scaling and tremor reduction [Video 1] Furthermore, the robotic arms of the system allow easier access to deep structures through smaller incisions. This opens the possibility of using the system for central lymphatic surgery of the thoracic duct, which will be the subject of further investigation.
Central lymphatic surgery may also become relevant in the treatment of patients after the Fontan procedure. This procedure is performed in children with a single functional ventricle. Lymphatic dysfunction in the Fontan circulation is among the postoperative complications and leads to plastic bronchitis and protein-losing enteropathy. The situation may be complex due to often elevated venous pressures in the Fontan circulation. However, in selected cases, lymphatic flow may have been mechanically interrupted by repetitive heart surgery and thoracic duct reconstruction may be a promising strategy to reestablish lymphatic flow and reduce symptoms. Current treatment strategies include lymphatic embolization and thoracic duct decompression[38]. A new approach could be the creation of an anastomosis between the thoracic duct and a nearby vein to redirect lymphatic drainage. However, against the background of the underlying disease with significantly impaired cardiac function and increased perioperative risks, the indication must be made with utmost caution and microsurgical treatment should only be offered in specialized centers.
CONCLUSION
There is an increasing number of reports with successful outcomes after thoracic duct-vein anastomoses in adults as well as in children with acquired or congenital central lymphatic lesions. Treatment success may vary, which is mainly attributed to the complex physiology of congenital central lymphatic anomalies with multiple sites of leakage and impaired peristalsis. Given the burden and the high morbidity of central lymphatic lesions, microsurgical reconstruction offers a chance of cure with a relatively low perioperative risk for patients.
DECLARATIONS
Authors’ contributionsMade substantial contributions to the design of the structure and content of the review: Grünherz L, Lindenblatt N
Availability of data and materialsNot applicable.
Financial support and sponsorshipNone.
Conflicts of interestNicole Lindenblatt acts as consultant and clinical advisor for Medical Microinstruments (MMI).
Ethical approval and consent to participateNot applicable.
Consent for publicationWritten informed consent for the publication of patient images was obtained.
Copyright© The Author(s) 2023.
REFERENCES
1. Gordon K, Varney R, Keeley V, et al. Update and audit of the St George's classification algorithm of primary lymphatic anomalies: a clinical and molecular approach to diagnosis. J Med Genet 2020;57:653-9.
2. Mäkinen T, Boon LM, Vikkula M, Alitalo K. Lymphatic malformations: genetics, mechanisms and therapeutic strategies. Circ Res 2021;129:136-54.
3. Kupferman ME, Patterson DM, Mandel SJ, LiVolsi V, Weber RS. Safety of modified radical neck dissection for differentiated thyroid carcinoma. Laryngoscope 2004;114:403-6.
4. Roh JL, Yoon YH, Park CI. Chyle leakage in patients undergoing thyroidectomy plus central neck dissection for differentiated papillary thyroid carcinoma. Ann Surg Oncol 2008;15:2576-80.
5. Lee YS, Kim BW, Chang HS, Park CS. Factors predisposing to chyle leakage following thyroid cancer surgery without lateral neck dissection. Head Neck 2013;35:1149-52.
6. Lee EW, Shin JH, Ko HK, Park J, Kim SH, Sung KB. Lymphangiography to treat postoperative lymphatic leakage: a technical review. Korean J Radiol 2014;15:724-32.
7. Ahn D, Sohn JH, Jeong JY. Chyle fistula after neck dissection: an 8-year, single-center, prospective study of incidence, clinical features, and treatment. Ann Surg Oncol 2015;22 Suppl 3:S1000-6.
8. Park I, Her N, Choe JH, Kim JS, Kim JH. Management of chyle leakage after thyroidectomy, cervical lymph node dissection, in patients with thyroid cancer. Head Neck 2018;40:7-15.
10. Lagarde SM, Omloo JM, de Jong K, et al. Incidence and management of chyle leakage after esophagectomy. Ann Thorac Surg 2005;80:449-54.
11. RochéRodríguez M, DiNardo JA. The lymphatic system in the fontan patient-pathophysiology, imaging, and interventions: what the anesthesiologist should know. J Cardiothorac Vasc Anesth 2022;36:2669-78.
12. Pieper CC, Feisst A, Schild HH. Contrast-enhanced Interstitial transpedal MR lymphangiography for thoracic chylous effusions. Radiology 2020;295:458-66.
13. Steven BR, Carey S. Nutritional management in patients with chyle leakage: a systematic review. Eur J Clin Nutr 2015;69:776-80.
14. Liviskie CJ, Brennan CC, McPherson CC, Vesoulis ZA. Propranolol for the treatment of lymphatic malformations in a neonate - a case report and review of literature. J Pediatr Pharmacol Ther 2020;25:155-62.
15. Hangul M, Kose M, Ozcan A, Unal E. Propranolol treatment for chylothorax due to diffuse lymphangiomatosis. Pediatr Blood Cancer 2019;66:e27592.
16. Ozeki M, Nozawa A, Yasue S, et al. The impact of sirolimus therapy on lesion size, clinical symptoms, and quality of life of patients with lymphatic anomalies. Orphanet J Rare Dis 2019;14:141.
17. Li D, March ME, Gutierrez-Uzquiza A, et al. ARAF recurrent mutation causes central conducting lymphatic anomaly treatable with a MEK inhibitor. Nat Med 2019;25:1116-22.
18. Swetman GL, Berk DR, Vasanawala SS, Feinstein JA, Lane AT, Bruckner AL. Sildenafil for severe lymphatic malformations. N Engl J Med 2012;366:384-6.
19. Morikawa K, Takenaga S, Hasumi J, et al. Retrograde transvenous lymphatic embolization for postoperative chylous ascites: a report of three cases and literature review. Radiol Case Rep 2020;15:1623-8.
20. Pieper CC, Hur S, Sommer CM, et al. Back to the future: lipiodol in lymphography-from diagnostics to theranostics. Invest Radiol 2019;54:600-15.
21. Schild HH, Naehle CP, Wilhelm KE, et al. Lymphatic interventions for treatment of chylothorax. Rofo 2015;187:584-8.
22. Schild HH, Pieper CC. Where have all the punctures gone? an analysis of thoracic duct embolizations. J Vasc Interv Radiol 2020;31:74-9.
23. Kylat RI, Witte MH, Barber BJ, Dori Y, Ghishan FK. Resolution of protein-losing enteropathy after congenital heart disease repair by selective lymphatic embolization. Pediatr Gastroenterol Hepatol Nutr 2019;22:594-600.
24. Lindenblatt N, Puippe G, Broglie MA, Giovanoli P, Grünherz L. Lymphovenous anastomosis for the treatment of thoracic duct lesion: a case report and systematic review of literature. Ann Plast Surg 2020;84:402-8.
25. Hong JPJ, Song S, Suh HSP. Supermicrosurgery: principles and applications. J Surg Oncol 2018;118:832-9.
26. Weissler JM, Cho EH, Koltz PF, et al. Lymphovenous anastomosis for the treatment of chylothorax in infants: a novel microsurgical approach to a devastating problem. Plast Reconstr Surg 2018;141:1502-7.
27. Miller TJ, Gilstrap JN, Maeda K, Rockson S, Nguyen DH. Correction of complete thoracic duct obstruction with lymphovenous bypass: a case report. Microsurgery 2019;39:255-8.
28. Yuan Y, Chen LQ, Zhao Y. Anastomosis between thoracic duct and azygos vein during esophagectomy: a novel technique with 3-year follow-up. World J Surg 2016;40:2984-7.
29. Rodi T, Tung Nguyen B, Fritsche E, Rajan G, Scaglioni MF. Direct repair of iatrogenic thoracic duct injury through lymphovenous anastomosis (LVA): a case report. J Surg Oncol 2020;121:224-7.
30. Feng J, Cheng J, Xiang F. Management of intractable pain in patients treated with hemorrhoidectomy for mixed hemorrhoids. Ann Palliat Med 2021;10:479-83.
31. Ciudad P, Chen HC, Bustos SS, et al. The deep inferior epigastric lymphatic cable flap connected to gastroepiploic lymph node flap for treatment of refractory chylous ascites: report of two cases. Microsurgery 2021;41:376-83.
32. Ishiura R, Mitsui K, Danno K, Banda CH, Inoue M, Narushima M. Successful treatment of large abdominal lymphatic malformations and chylous ascites with intra-abdominal lymphovenous anastomosis. J Vasc Surg Venous Lymphat Disord 2021;9:499-503.
33. Taghinia AH, Upton J, Trenor CC 3rd, et al. Lymphaticovenous bypass of the thoracic duct for the treatment of chylous leak in central conducting lymphatic anomalies. J Pediatr Surg 2019;54:562-8.
34. Othman S, Azoury SC, Klifto K, Toyoda Y, Itkin M, Kovach SJ. Microsurgical thoracic duct lymphovenous bypass in the adult population. Plast Reconstr Surg Glob Open 2021;9:e3875.
35. Lindenblatt N, Gutschow CA, Vetter D, et al. Lympho-venous anastomosis for the treatment of congenital and acquired lesions of the central lymphatic system: a multidisciplinary treatment approach. Eur J Plast Surg 2022;45:841-9.
36. Barbon C, Grünherz L, Uyulmaz S, Giovanoli P, Lindenblatt N. Exploring the learning curve of a new robotic microsurgical system for microsurgery. JPRAS Open 2022;34:126-33.
37. Lindenblatt N, Grünherz L, Wang A, et al. Early Experience using a new robotic microsurgical system for lymphatic surgery. Plast Reconstr Surg Glob Open 2022;10:e4013.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Grünherz L, Lindenblatt N. Central lymphatic surgery. Plast Aesthet Res 2023;10:20. http://dx.doi.org/10.20517/2347-9264.2023.24
AMA Style
Grünherz L, Lindenblatt N. Central lymphatic surgery. Plastic and Aesthetic Research. 2023; 10: 20. http://dx.doi.org/10.20517/2347-9264.2023.24
Chicago/Turabian Style
Grünherz, Lisanne, Nicole Lindenblatt. 2023. "Central lymphatic surgery" Plastic and Aesthetic Research. 10: 20. http://dx.doi.org/10.20517/2347-9264.2023.24
ACS Style
Grünherz, L.; Lindenblatt N. Central lymphatic surgery. Plast. Aesthet. Res. 2023, 10, 20. http://dx.doi.org/10.20517/2347-9264.2023.24
About This Article
Special Issue
Copyright
Data & Comments
Data
 Cite This Article 12 clicks
Cite This Article 12 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.