Nanofibrillar collagen scaffolds for lymphedema treatment: current applications and future directions
Abstract
Aim: Biosynthetic scaffolds represent cutting-edge therapeutic efforts for secondary lymphedema. In particular, nanofibrillar collagen scaffolds have shown efficacy in both preclinical and clinical contexts, and there has been growing interest in these scaffolds in recent years. This study systematically reviewed the current literature on nanofibrillar collagen scaffolds for lymphedema treatment to synthesize findings and highlight areas for further research.
Methods: This was a systematic scoping review of the literature on nanofibrillar collagen scaffolds for lymphedema treatment.
Results: Upon review of the literature, 32 relevant articles were identified, of which seven articles specifically investigating nanofibrillar collagen scaffolds were selected for inclusion. Of these articles, three investigated scaffold placement in small or large animal models, while four were clinical investigations ranging from case reports to retrospective cohort studies. Across all studies, scaffold implantation was associated with significant improvement in lymphedema symptoms compared to untreated controls, especially when used in combination with physiologic microsurgical procedures such as vascularized lymph node transfer. However, even when used alone or in combination with lymph node fragments, subcutaneous placement of these scaffolds improved lymphedema symptoms. Additionally, in a rodent model of lymphedema, scaffold placement at the time of lymph node harvest forestalled the development of lymphedema, highlighting the preventative capacity of these scaffolds as well.
Conclusion: Nanofibrillar collagen scaffolds have been demonstrated to effectively treat and/or prevent secondary lymphedema in both preclinical and clinical investigations. Ultimately, these scaffolds represent a promising intersection of tissue engineering and lymphedema therapy, and further clinical investigation is warranted.
Keywords
INTRODUCTION
Secondary lymphedema is a relatively common and highly morbid iatrogenic complication after cancer resection, especially in those who undergo concomitant radiation therapy[1]. In fact, amongst breast cancer patients, some studies report secondary lymphedema incidence rates of greater than 50%[2]. Thus, this disease poses a substantial clinical and psychosocial burden amongst cancer survivors. Although diagnosis and treatment of lymphedema have improved over the years, sustainable, replicable therapy has remained a challenge.
Several techniques for the treatment of lymphedema have been developed, primarily aimed at redirecting interstitial fluid back into lymphaticovenous channels to restore lymphatic flow. These treatments range from conservative measures involving mechanical compression (i.e., complete decongestive therapy) to microsurgical techniques designed to transpose lymphatic networks (i.e., vascularized lymph node transfer) or to redirect lymphatic flow into the venous system (i.e., lymphovenous anastomosis)[3]. More recently, biomaterials-based treatments have emerged with a focus on augmenting/accelerating lymphatic regeneration. Such treatments include nanofibrillar collagen scaffolds, which mimic the collagen extracellular matrix in vasculature and can be seeded with stem cells or growth factors to help stimulate lymphangiogenesis[4].
As survival improves amongst cancer patients, management of sequelae such as secondary lymphedema has become paramount in ensuring long-term quality of life. There has been a recent surge in biomaterials research for lymphedema treatment, with investigations spanning the gamut from preclinical studies through clinical trials. This paper systematically reviews the current literature on biosynthetic nanofibrillar collagen scaffolds for lymphedema treatment by reviewing recent innovations in the field and exploring areas for further research.
METHODS
This was a systematic scoping review of the English-language literature investigating nanofibrillar collagen scaffolds for the treatment of secondary lymphedema. A structured literature search was performed with the MeSH terms listed in the Supplementary Tables 1-4, using databases including PubMed, MEDLINE, EMBASE, Scopus, the Cochrane Central Register of Controlled Trials, and Web of Science. Covidence management software (Melbourne, Australia) was utilized to screen, perform quality assessments, and extract data from included literature. Studies were selected using predefined inclusion criteria created using a Population, Intervention, Comparison, Outcome, Timing, and Setting (PICOTS) framework. Inclusion criteria were as follows: (1) English-language; (2) original research article (i.e., not a review article or meta-analysis) published after 1990; and (3) primarily investigating nanofibrillar collagen scaffolds for secondary lymphedema treatment (including preclinical, translational, and clinical investigations). Reference sections of articles meeting study criteria were also reviewed to identify any further relevant articles for study inclusion.
The study workflow was designed according to PRISMA guidelines[5]. Two independent study team members screened article titles, abstracts, and full texts for every article identified through a comprehensive literature search. Only articles primarily investigating nanofibrillar collagen scaffolds for lymphedema treatment were selected for final inclusion in the review. Any discrepancies in screening results were resolved through reviewer consensus. Two independent team members assessed the risk of bias for each article included in the final study cohort using the validated Risk of Bias in Non-Randomized Studies of Interventions (ROBINS-I) scale for clinical work and the SYRCLE’s risk of bias tool for animal studies[6,7]. Study objectives, design, interventions, results, and conclusions were extracted for each included study. Study data were tabulated to synthesize the literature on the use of biosynthetic nanofibrillar collagen scaffolds for lymphedema treatment.
RESULTS
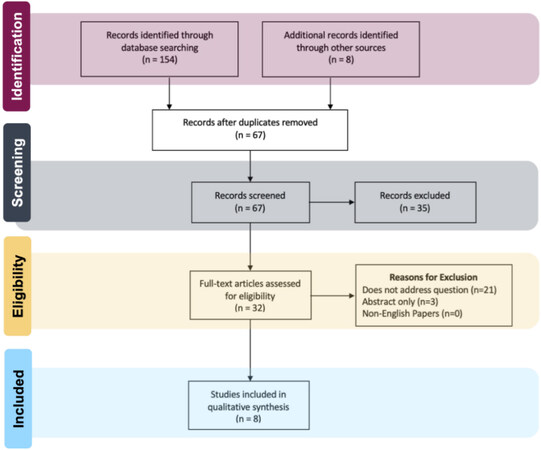
In total, 32 English language articles were identified from the initial query, of which eight articles specifically investigating nanofibrillar collagen scaffolds for secondary lymphedema were selected for inclusion in the final review. Figure 1 demonstrates the algorithm for the selection of the final set of articles included in this study.
All included articles were either preclinical investigations of biosynthetic nanofibrillar collagen scaffolds for lymphedema treatment in animal models of lymphedema, or clinical cohort studies of these scaffolds in human subjects. The overall risk of bias was moderate for two studies and low for six studies
DISCUSSION
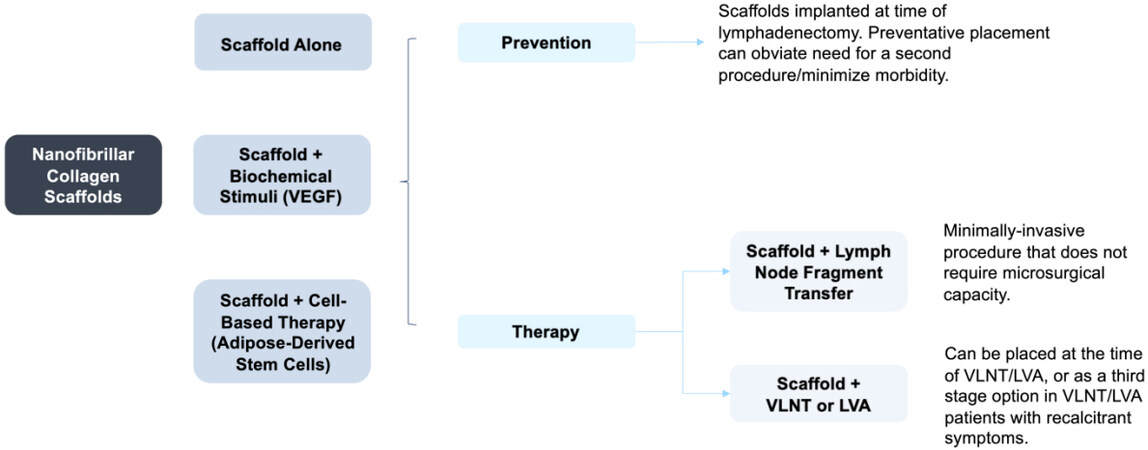
Novel tissue engineering efforts in lymphedema treatment have focused on designing scaffolds to guide and enhance lymphangiogenesis to regenerate lymphatic channels after iatrogenic injury. A number of biomaterials have been studied in the context of promoting lymphatic regeneration, ranging from endothelial cell-seeded polyglycolic acid scaffolds, fibrin/fibrin-collagen matrices, and fibrin hydrogels to bioengineered dermal grafts/acellular dermal matrices and decellularized adipose tissue matrices[8-11]. In particular, nanofibrillar collagen scaffolds have demonstrated particular efficacy in enhancing lymphangiogenesis[4]. From a review of both preclinical and clinical investigations, these nanofibrillar biosynthetic collagen scaffolds have been demonstrated to improve outcomes in secondary lymphedema across both preventative and therapeutic contexts [Figure 2].
Figure 2. Utility of nanofibrillar biosynthetic scaffolds for lymphedema. VEGF: Vascular endothelial growth factor; VLNT: vascularized lymph node transfer; LVA: lymphaticovenous anastomosis.
Biosynthetic scaffolds: background
Lymphatic vessels have a unique architecture that is challenging to recapitulate[12]. A current focus of tissue engineering for lymphedema treatment involves the fabrication of biosynthetic scaffolds, which can be implanted in affected extremities to encourage lymphangiogenesis. These scaffolds are designed to function as three-dimensional templates for endothelial cell proliferation by acting as analogues to the extracellular matrix found in the native lymphatic vasculature. The biodegradable scaffolds are designed to be replaced by functional lymphatic channels over time. Furthermore, they can be used in combination with pro-lymphangiogenic growth factors or cell-based therapy by seeding the scaffold with growth factors or stem cells known to be involved in lymphangiogenesis[13,14].
Multiple biomaterials have been investigated as scaffolds for lymphangiogenesis, including polyglycolic acid/polylactic acid, human acellular dermal matrix, decellularized adipose tissue matrix, fibrin matrices in arterio-venous loop systems, and type 1 collagen nanofibrils[11,13,15-19]. In particular, nanofibrillar collagen scaffolds, marketed as BioBridge (Fibralign Corporation, Union City, CA), have shown promise in enhancing lymphatic regeneration when used alone or when seeded with stem cells. These scaffolds are a class II device cleared through the 510(K) pathway, composed of medical grade type 1 monomeric collagen fibrils that are aligned to create membranes with high mechanical tensile strength and a stable structure. These scaffolds are fabricated into thin, ribbon-like structures that are implanted subcutaneously to bypass areas of lymphatic obstruction caused by scar tissue/fibrosis.
Given their biomimetic properties that guide cellular organization and enhance cell survival, nanofibrillar collagen scaffolds have multiple uses in regenerative medicine, ranging from nerve and vascular regeneration (e.g., neovascularization in ischemic limbs) to bone tissue engineering[20-22]. With regards to lymphedema, specifically, BioBridge scaffolds mimic native extracellular matrices, enabling endothelial cell infiltration and remodeling to recreate lymphatic vasculature. Furthermore, the nanofibrillar structure of these scaffolds guides directional local interstitial flow, which is known to be a factor in stimulating lymphangiogenesis[23]. The nanofibrillar collagen encourages endothelial cell cytoskeletal reorganization along the direction of the scaffold and provides support to enhance endothelial cell survival[24]. Ultimately, endothelial cells migrate into the scaffold, attach, and proliferate, leading to the directional development of mature lymphatic vasculature.
Nanofibrillar collagen scaffolds have been used alone and in combination with other therapies. When implanted at the time of vascularized lymph node transfer, for instance, nanofibrillar collagen scaffolds have been shown to accelerate the engraftment of lymphatic tissue by increasing endothelial cell migration and formation of lymphatic vasculature[25-27]. Lymph node transfer is thought to stimulate lymphangiogenesis in the surrounding tissue, and the scaffold augments this process by providing soft tissue support for the directional growth of lymphatic channels, as previously described[28]. However, BioBridge scaffolds have also been successfully used alone-the nanofibrillar structure of these scaffolds holds intrinsic capacity to engender lymphangiogenesis through the aforementioned mechanisms (e.g., stimulating flow of interstitial fluid, encouraging migration of endothelial cells, and enhancing expression of lymphangiogenetic factors in the surrounding milieu such as vascular endothelial growth factor)[29,30]. This highlights the immense potential that biomaterial design and tissue engineering hold for lymphedema treatment, as optimally-designed scaffolds can act in a standalone capacity to enhance lymphatic regeneration[31].
Nanofibrillar collagen scaffolds: preclinical investigations
Preclinical investigations of nanofibrillar collagen scaffolds have spanned both small and large animal models [Table 1]. In a rat model of acquired lymphedema, implantation of the BioBridge scaffold seeded with adipose-derived stem cells demonstrated significant positive effects when utilized in a preventative capacity or as a treatment in animals with established disease[32]. In this study, rodents underwent surgical excision of hind limb lymphatics and were assigned into either an untreated control group or one of two treatment groups - (1) BioBridge placement prior to irradiation (i.e., preventative placement); and (2) implantation of BioBridge scaffolds seeded with adipose-derived stem cells after lymphedema symptoms were established (i.e., therapeutic placement). When BioBridge was implanted pre-emptively at the time of inguinal and popliteal lymph node excision, rats did not develop hind limb lymphedema in the affected extremity, unlike untreated controls, as determined by computed tomography-based volumetric analysis at the 1-month postoperative timepoint. Additionally, when BioBridge scaffolds seeded with stem cells were implanted in rodents with established lymphedema, affected limb volume was significantly reduced compared to untreated controls at 4 months postoperatively, with enhanced lymphatic regeneration confirmed by near-infrared fluoroscopy.
Summary of preclinical investigations
| Study | Objectives | Study design | Treatments | Number of animals | Timeline/Duration | Study outcomes |
| Small animal | ||||||
| Nguyen et al., 2022[32] | To investigate the efficacy of BioBridge implantation both preventatively and as a treatment in a rodent model of acquired lymphedema. Outcomes were measured using CT-based volumetric analysis and near-infrared fluoroscopy to detect lymphatic regeneration | Randomized Factorial Design (2 treatment groups) | (1) Untreated controls (2) BioBridge after lymphadenectomy but prior to radiation (preventive) (3) BioBridge + autologous adipose-derived stem cells (treatment) | n = 7 prevention group; n = 5 treatment group | BioBridge was implanted immediately in the preventive group, and 1 month after the establishment of lymphedema in the treatment group, study data were collected up to 4 months after scaffold implantation | BioBridge implantation at the time of lymph node excision prevented lymphedema development. BioBridge seeded with stem cells also had therapeutic effects in rodents with established lymphedema, with demonstrated regeneration of lymphatic vasculature |
| Large animal | ||||||
| Hadamitzky et al., 2016[33] | To investigate the efficacy of BioBridge scaffold placement +/- concurrent vascularized lymph node transfer in a porcine model of acquired lymphedema. Outcomes were assessed using bioimpedance, histologic evaluation, and computed tomography imaging of lymphatic vessels in the treated limb | Randomized Factorial Design (2 treatment groups) | (1) Untreated controls (2) BioBridge + VEGF-C (3) BioBridge + lymph node fragments | n = 4 control; n = 4 BioBridge + VEGF-C; n = 8 BioBridge + lymph node fragments | BioBridge was implanted 3 months after establishment of lymphedema; study data were collected up to 3 months after scaffold implantation | BioBridge treatment with or without lymph node transfer significantly improved bioimpedance ratios and increased quantifiable lymphatic collectors in the treated area, indicating targeted regeneration of functional lymphatic vessels. VEGF-C, on the other hand, was found to hinder directional lymphangiogenic sprouting |
Nanofibrillar collagen scaffolds have also demonstrated promising results in large animal models. Hadamitzky et al. investigated the BioBridge scaffold in a validated porcine model of secondary lymphedema, which is generated by surgically resecting hindlimb lymphatics and delivering a single dose of radiotherapy to the groin[33]. In this study, animals were randomized to one of three groups - (1) control (no treatment); (2) BioBridge with autologous lymph node fragment transfer; or (3) BioBridge supplemented with vascular endothelial growth factor-C (VEGF-C), a growth factor known to enhance lymphatic sprouting, at a concentration (1.5 micrograms/mL) that optimized VEGF-C loading and release profiles[34]. Three-month post-treatment outcomes were investigated using bioimpedance ratios and by CT contrast lymphangiography. This study demonstrated that BioBridge implantation significantly enhanced lymphatic regeneration when placed alone or in combination with autologous lymph node fragment transfer. Animals treated with BioBridge demonstrated a significantly greater density of lymphatic vessels. In fact, the highest density of lymphatic vessels in treated animals was found within 100 microns of the scaffold, demonstrating the specific impact that the scaffold had on augmenting lymphatic regeneration. Upon computed tomography imaging and bioimpedance testing, the BioBridge treatment group with concurrent autologous lymph node fragment transfer demonstrated functional improvement in lymphedema symptoms compared to the control group. In experimental groups treated with VEGF-C impregnated scaffolds, however, it was found that exogenous VEGF-C resulted in nonfunctional lymphangiogenesis. The presence of growth factor distributed uniformly along the length of the scaffold obscured the directionality of lymphatic regeneration, resulting in ineffectual lymphangiogenesis.
Nanofibrillar collagen scaffolds: clinical investigations
Nanofibrillar collagen scaffolds have also been investigated in humans, with preliminary results demonstrating the safety of scaffold placement as well as success in improving lymphedema symptoms [Table 2]. Study eligibility criteria are reported in Table 2 - including studies that investigated BioBridge placement in lymphedema patients across a variety of stages (stage I-III), as both a primary treatment and a secondary procedure in patients who had already undergone prior physiologic therapy (e.g., LVA, VLNT). Nguyen et al. investigated delayed implantation of BioBridge scaffolds in secondary lymphedema patients who had undergone prior lymphaticovenous anastomosis and/or vascularized lymph node transfer[35]. Included patients were largely stage 1 to stage 2 lymphedema patients with a unilaterally affected extremity, who either had a suboptimal response to their initial physiologic procedure or desired further improvement in their lymphedema symptoms. After scar release and liposuction, if indicated, BioBridge scaffolds were tunneled subcutaneously to create a connection between intact native lymphatic tissue and the site of the prior lymphaticovenous anastomosis or vascularized lymph node transfer. Patients in the BioBridge cohort had a significantly greater reduction in the volume of the affected limb compared to historical controls (111% vs. 70% edema reduction, respectively), with lymphatic mapping demonstrating evidence of lymphangiogenesis and decreased dermal backflow in the BioBridge cohort. Furthermore, both surgical subgroups (lymphaticovenous anastomosis and vascularized lymph node transfer) demonstrated positive results with BioBridge placement, although a greater treatment response was noted in the vascularized lymph node transfer group compared to the lymphaticovenous anastomosis group (7.6-fold versus 3.5-fold increase in edema reduction, respectively). These successful results were sustained upon long-term follow-up - more than 75% of patients who underwent BioBridge implantation maintained normal limb volumes at an average of 29 months post-implantation.
Summary of clinical investigations
| Study | Objectives | Study design | Study population/eligibility criteria | Treatments/Number of subjects | Timeline/Follow up | Study outcomes |
| Nguyen et al., 2021[35] | To investigate the utility of BioBridge scaffolds in augmenting the effects of LVA and/or VLNT for secondary lymphedema. Cohorts were compared based on limb volume and indocyanine green fluorescence lymphatic mapping | Retrospective cohort investigation, 2016-2019 | Patients with stage 1 to stage 3 secondary lymphedema are patients with a unilaterally affected extremity, who had undergone prior LVA and/or VLNT | n = 18 BioBridge cohort; n = 11 retrospective controls | BioBridge placed on average 16.7 months (range, 1-72 months) after LVA/VLNT; Mean follow-up was 29 months | Limb volume was significantly reduced in the BioBridge cohort, with those who underwent prior VLNT demonstrating more pronounced results. These results were sustained upon longitudinal follow-up |
| Hadamitzky et al., 2017[40] | To investigate the efficacy of BioBridge placement in combination with autologous lymph node fragment transfer, with or without adipose-derived stromal cells | Prospective cohort investigation | Patients with secondary lymphedema of a unilateral extremity | n = 8 BioBridge + lymph node fragment transfer (5 with scaffolds alone, 3 with adipose stromal cells); n = 4 lymph node fragment transfer | BioBridge and lymph node fragments were implanted concurrently, time from lymphedema diagnosis was not specified. Follow-up to 6 months post-implantation was reported | Use of BioBridge resulted in a 20% average limb volume reduction, compared to 1% in those treated with lymph node fragment transfer alone |
| Deptula et al., 2022[36] | To investigate BioBridge efficacy in patients with advanced secondary lymphedema and to create a treatment algorithm for BioBridge placement | Retrospective cohort investigation | Patients with late stage 2 to stage 3 secondary lymphedema are patients with a unilaterally affected extremity who had undergone prior LVA and/or VLNT | n = 14 BioBridge cohort | Patients were considered for BioBridge placement 1-2 years after liposuction/physiologic procedure. Follow-up was at least 24 months | In patients with excess fluid volume after liposuction and physiologic treatment (LVA, VLNT), subsequent BioBridge placement normalized limb volumes, with sustained results more than 2 years after surgery |
| Inchauste et al., 2020[39] | To investigate BioBridge with concurrent VLNT in a lymphedema patient with peripheral vascular disease | Retrospective case report | Patient with stage 3 lower extremity secondary lymphedema, with concurrent neuropathy and femoral artery thrombosis | n = 1 | Patient was treated with VLNT and BioBridge ~30 years after the onset of lymphedema symptoms; outcomes at 3 months post-implantation were reported | BioBridge placement resulted in volume reduction, improved neuropathic pain, and improved ambulation in the affected extremity |
| Dionyssiou et al., 2021[41] | To propose an algorithmic approach to concurrent breast reconstruction and lymphedema treatment with vascularized lymph node transfer and scaffold placement | Retrospective cohort investigation | Partial or total mastectomy patients with stage 1-3 lymphedema refractory to medical therapy | n = 69 | BioBridge implanted at the time of delayed breast/lymphatic reconstruction; mean time since lymphedema diagnosis not reported; mean follow-up was 4 years | Simultaneous breast and lymphedema reconstruction with lymph node transfer and scaffold placement was effective in achieving sustained volume reduction, reducing infections, and improving patient satisfaction |
Retrospective clinical investigations have studied secondary BioBridge placement in secondary lymphedema patients with more advanced disease, intending to create treatment algorithms to optimize outcomes[36,37]. Brazio et al. retrospectively reviewed outcomes of patients with stage II-III lymphedema undergoing physiologic procedures versus liposuction, with downstream scaffold placement in some cases[37]. They found that patients with predominantly non-pitting lymphedema benefitted most from liposuction prior to physiologic procedure/scaffold placement, while those with primarily pitting edema were best treated with physiologic procedure first and liposuction as a possible second stage[37]. Building on this study, Deptula et al. investigated outcomes in late stage 2 to stage 3 secondary lymphedema patients who underwent prior physiologic procedures to devise an algorithm that identifies ideal candidates for downstream BioBridge placement[36]. All included patients were treated with a proposed “triple therapy” involving initial debulking with liposuction, followed by a physiologic procedure (lymphaticovenous anastomosis or vascularized lymph node transfer) and then BioBridge placement. BioBridge placement as part of this “triple” therapy was found to have the greatest impact in patients with persistent excess limb volume due to continued fluid accumulation after lymphaticovenous anastomosis or vascularized lymph node transfer. In fact, BioBridge placement in appropriately selected patients completely normalized limb volume in the affected extremity, with sustained results noted at the two-year postoperative timepoint from the initial BioBridge placement. Unlike standard debulking therapies such as liposuction alone, which require ongoing compression therapy to prevent relapse, this triple therapy recreates lymphatic flow and thus allows patients to ultimately wean compression garments and achieve endogenous volume control in the affected extremity through the physiologic restoration of lymphatic circulation[36,38].
While the previously described work demonstrated successful placement of BioBridge as a delayed therapy after a physiologic procedure, a recent case report in a patient with stage III right lower extremity secondary lymphedema has demonstrated that BioBridge implantation is also successful in normalizing limb volume when implanted concurrently with vascularized lymph node transfer[39]. Notably, this patient also had radiation-related peripheral vascular disease and peripheral neuropathy in the affected limb, and had undergone prior revascularization with a saphenous vein graft due to radiation-induced femoral artery thrombosis. In this patient, BioBridge scaffolds were placed subcutaneously after scar release at the time of vascularized lymph node transfer to provide soft tissue support and to bridge the lymph node transfer to healthy native lymph tissue. Ultimately, vascularized lymph node transfer in combination with BioBridge placement resulted in sustained limb volume reduction, improved neuropathic pain, and improved ambulation three months post-procedurally, demonstrating that nanofibrillar collagen scaffolds can also be safely placed at the time of microsurgical physiologic lymphedema procedures.
Preliminary data in secondary lymphedema patients have also demonstrated that BioBridge scaffolds seeded with adipose-derived stromal cells in combination with non-vascularized autologous lymph node fragment transfer resulted in sustained improvement in lymphedema symptoms[40]. A majority of patients treated with seeded BioBridge scaffolds and lymph node fragment transfer demonstrated substantial volume reduction in the affected extremity at 6 months postoperatively (mean volume reduction reported was 20%, with 1/3 of the patients reporting complete normalization of limb volumes), compared to a 1% volume reduction in controls who received lymph node fragment transfer alone. These results highlight the specific, synergistic effect of BioBridge scaffolds in enhancing lymphangiogenesis, given that lymph node fragment transfer alone was not enough to create measurable improvements in lymphedema symptoms.
Finally, Dionyssiou et al. (2021) investigated simultaneous breast and lymphedema reconstruction[41]. In this study, collagen scaffolds were subcutaneously inserted in the upper limb, in combination with pedicled or free vascularized lymph node transfer, to enhance lymphangiogenesis during partial or total breast reconstruction. Treated patients had fewer episodes of infection, significantly reduced pain and heaviness, significantly improved overall function, and evidence of dermal backflow reduction at 1 year postoperative follow-up. No complications specifically related to collagen scaffold placement were reported.
Nanofibrillar collagen scaffolds in the context of current lymphedema treatment
Regenerative medicine holds immense promise for secondary lymphedema and represents the cutting-edge therapies in this field that have the potential for curative treatment[13,42,43]. Tissue engineering efforts with nanofibrillar collagen scaffolds offer a number of advantages over current standard-of-care therapies for secondary lymphedema as it provides a biomaterial structure that can mimic native extracellular matrix and drive lymphatic regeneration in synergy with cellular and biochemical growth factors[44]. Unlike physiotherapy with drainage and compression or ablative surgical procedures, these scaffolds have the potential to obviate the need for repeat surgery or lifelong therapy, and they directly address the pathophysiology of the disease rather than simply providing symptomatic treatment[15]. Compared to physiologic procedures (e.g., vascularized lymph node transfer, lymphaticovenous anastomosis), nanofibrillar collagen scaffolds are minimally invasive, placed subcutaneously in affected limbs to encourage lymphatic flow across scar tissue, and do not require microsurgical anastomoses or a donor site.
Ultimately, nanofibrillar collagen scaffolds have been demonstrated to stimulate lymphangiogenesis when used alone, in combination with cell-based therapy, and in combination with lymph node fragment transfer or physiologic procedures such as lymphaticovenous anastomosis and vascularized lymph node transfer. Furthermore, the use of BioBridge offers patients an adjunct procedure that can enhance results beyond a physiologic procedure alone, even in late-stage secondary lymphedema, without incurring additional donor site morbidity as would an additional lymph node transfer[25]. Overall, while the specific indications for BioBridge are still under investigation, this technology has demonstrated efficacy across several lymphedema populations (i.e., primary therapy versus secondary therapy after previous physiologic procedure) by helping to improve lymphedema symptoms and engendering targeted, functional lymphangiogenesis. However, it should be noted that BioBridge therapy is thought to confer the greatest efficacy in patients with excess fluid volume, as it aims to divert fluid back into lymphatic circulation. Thus, for patients with severe, late-stage lymphedema and excess fibrofatty tissue, the use of this technology as a primary or standalone therapy may be limited, and they may prefer to benefit from surgical debulking. With regards to contraindications, those with allergic or anaphylactic reactions to the materials in the BioBridge scaffold should not undergo scaffold implantation, and most included studies suggest that this scaffold should not be implanted in infected fields[36]. Those with evidence of cellulitis/soft tissue infection in the affected extremity should first be treated with antibiotics prior to undergoing lymphedema surgery.
It is important to note that BioBridge represents a physiologic intervention that can be undertaken even in clinical settings without microsurgical/supermicrosurgical capacity. This is especially encouraging for the treatment of secondary lymphedema in low-resource settings when considering the data from
Future directions
Nanofibrillar collagen biosynthetic scaffolds have evolved out of a need to improve outcomes in patients with acquired lymphedema. While current investigations have been largely observational, multi-center, prospective randomized controlled trials are necessary to truly evaluate the efficacy of these scaffolds as a viable treatment for secondary lymphedema. Currently, the clinical trial is underway comparing vascularized lymph node transfer with BioBridge placement to vascularized lymph node transfer alone. Further clinical trials should also investigate the preventive capacity of these scaffolds. There are many efforts underway (e.g., LYMPHA) investigating the utility of microsurgical lymphedema treatments undertaken in a preventative context[45]. Future work should investigate the efficacy of pre-emptive scaffold placement in patients undergoing lymph node dissection to forestall the development of lymphedema, especially given promising preclinical results with preventative scaffold placement in rodent models of lymphedema.
Additionally, further studies from a tissue engineering perspective are needed to optimize nanofibrillar collagen scaffolds and maximize their potential for lymphangiogenesis (e.g., supplementing the scaffolds with biochemical stimuli such as vascularized endothelial growth factor, or seeding the scaffolds with stem cells). While most current efforts focus on recreating lymphatic vasculature, future work should also investigate the feasibility of engineering constructs to regenerate the lymph node itself to obviate the need for lymph node transfers[15].
As previously described, nanofibrillar collagen scaffolds represent a viable physiologic therapy for secondary lymphedema that is minimally invasive and does not require microsurgical technique. Further work should investigate the relative cost-effectiveness of using these scaffolds in secondary lymphedema patients to better understand their utility in high-volume lymphedema centers as well as their applicability to low-resource settings. Additionally, understanding the cost-effectiveness of these scaffolds can help inform reimbursement and coverage for these procedures, as acquired lymphedema remains a substantial survivorship issue amongst cancer patients[32].
In conclusion, this article reviewed novel tissue engineering efforts for the treatment of secondary lymphedema, with a particular focus on nanofibrillar collagen scaffolds. Overall, these scaffolds have demonstrated promise in augmenting lymphangiogenesis upon both preclinical and clinical testing, and they have been demonstrated to improve secondary lymphedema outcomes when used both preventatively and therapeutically.
DECLARATIONS
Authors’ contributionsContributed to conception and design, acquisition, analysis, interpretation of data, manuscript writing, and final approval of manuscript: Yesantharao PS, Nguyen DH
Availability of data and materialsStudy articles and data are available at reasonable request of the corresponding author.
Financial support and sponsorshipNone.
Conflicts of interestDr. Dung H. Nguyen is the Principal Investigator of ongoing clinical trials of BioBridge in lymphedema patients. Both authors declared that there are no conflicts of interest.
Ethical approval and consent to participateNot applicable.
Consent for publicationNot applicable.
Copyright© The Author(s) 2022.
Supplementary MaterialsREFERENCES
1. Cormier JN, Askew RL, Mungovan KS, Xing Y, Ross MI, Armer JM. Lymphedema beyond breast cancer: a systematic review and meta-analysis of cancer-related secondary lymphedema. Cancer 2010;116:5138-49.
2. Armer JM, Stewart BR. Post-breast cancer lymphedema: incidence increases from 12 to 30 to 60 months. Lymphology 2010;43:118-27.
3. Chang DW, Masia J, Garza R 3rd, Skoracki R, Neligan PC. Lymphedema: surgical and medical therapy. Plast Reconstr Surg 2016;138:209S-18S.
4. Rochlin DH, Inchauste S, Zelones J, Nguyen DH. The role of adjunct nanofibrillar collagen scaffold implantation in the surgical management of secondary lymphedema: Review of the literature and summary of initial pilot studies. J Surg Oncol 2020;121:121-8.
5. Welch V, Petticrew M, Tugwell P, et al. PRISMA-Equity Bellagio group. PRISMA-Equity 2012 extension: reporting guidelines for systematic reviews with a focus on health equity. PLoS Med 2012;9:e1001333.
6. Sterne JA, Hernán MA, Reeves BC, et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 2016;355:i4919.
7. Hooijmans CR, Rovers MM, de Vries RB, Leenaars M, Ritskes-Hoitinga M, Langendam MW. SYRCLE’s risk of bias tool for animal studies. BMC Med Res Methodol 2014;14:43.
8. Dai Tt, Jiang Zh, Li Sl, et al. Reconstruction of lymph vessel by lymphatic endothelial cells combined with polyglycolic acid scaffolds: a pilot study. J Biotechnol 2010;150:182-9.
9. Helm CL, Zisch A, Swartz MA. Engineered blood and lymphatic capillaries in 3-D VEGF-fibrin-collagen matrices with interstitial flow. Biotechnol Bioeng 2007;96:167-76.
10. Zhang Q, Wu Y, Schaverien MV, Hanson SE, Chang EI, Butler CE. Abstract 128: engineering lymphatic vessels for secondary lymphedema treatment. Plast Reconstr Surg Glob Open 2020;8:85-6.
11. Wong AK, Schonmeyer BH, Singh P, Carlson DL, Li S, Mehrara BJ. Histologic analysis of angiogenesis and lymphangiogenesis in acellular human dermis. Plast Reconstr Surg 2008;121:1144-52.
12. Asaad M, Hanson SE. Tissue engineering strategies for cancer-related lymphedema. Tissue Eng Part A 2021;27:489-99.
13. Sung CJ, Gupta K, Wang J, Wong AK. Lymphatic tissue bioengineering for the treatment of postsurgical lymphedema. Bioengineering (Basel) 2022;9:162.
14. Kolarzyk AM, Wong G, Lee E. Lymphatic tissue and organ engineering for in vitro modeling and in vivo regeneration. Cold Spring Harb Perspect Med ;2022:a041169.
15. Neßbach P, Aitzetmüller MM. Translational challenges: lymph node tissue engineering. In: Duscher D, Shiffman MA, editors. Regenerative medicine and plastic surgery. Cham: Springer International Publishing; 2019. p. 293-301.
16. Campbell KT. Alginate biomaterial delivery systems for potential therapeutic lymphangiogenic applications: University of California, Davis; 2020. Available from: https://www.proquest.com/openview/aebaf4a9446960c4819d523f3c8080fb/1?pq-origsite=gscholar&cbl=18750&diss=y [Last accessed on 1 Nov 2022].
17. Kanapathy M, Kalaskar D, Mosahebi A, Seifalian AM. Development of a tissue-engineered lymphatic graft using nanocomposite polymer for the treatment of secondary lymphedema. Artif Organs 2016;40:E1-11.
18. Hooks JST, Bernard FC, Cruz-Acuña R, et al. Synthetic hydrogels engineered to promote collecting lymphatic vessel sprouting. Biomaterials 2022;284:121483.
19. Alderfer L, Hall E, Hanjaya-Putra D. Harnessing biomaterials for lymphatic system modulation. Acta Biomater 2021;133:34-45.
20. Nakayama KH, Hong G, Lee JC, et al. Aligned-braided nanofibrillar scaffold with endothelial cells enhances arteriogenesis. ACS Nano 2015;9:6900-8.
21. Nakayama KH, Alcazar C, Yang G, et al. Rehabilitative exercise and spatially patterned nanofibrillar scaffolds enhance vascularization and innervation following volumetric muscle loss. NPJ Regen Med 2018;3:16.
22. Marelli B, Ghezzi CE, Barralet JE, Boccaccini AR, Nazhat SN. Three-dimensional mineralization of dense nanofibrillar collagen-bioglass hybrid scaffolds. Biomacromolecules 2010;11:1470-9.
23. Boardman KC, Swartz MA. Interstitial flow as a guide for lymphangiogenesis. Circ Res 2003;92:801-8.
24. Huang NF, Okogbaa J, Lee JC, et al. The modulation of endothelial cell morphology, function, and survival using anisotropic nanofibrillar collagen scaffolds. Biomaterials 2013;34:4038-47.
25. McLaughlin SA, DeSnyder SM, Klimberg S, et al. Considerations for clinicians in the diagnosis, prevention, and treatment of breast cancer-related lymphedema, recommendations from an expert panel: part 2: preventive and therapeutic options. Ann Surg Oncol 2017;24:2827-35.
27. Lai ES, Huang NF, Cooke JP, Fuller GG. Aligned nanofibrillar collagen regulates endothelial organization and migration. Regen Med 2012;7:649-61.
28. Shuck J, Schaverien MV, Chang EI. Discussion: nanofibrillar collagen scaffold enhances edema reduction and formation of new lymphatic collectors after lymphedema surgery. Plast Reconstr Surg 2021;148:1394-5.
29. Schaverien MV, Aldrich MB. New and emerging treatments for lymphedema. Semin Plast Surg 2018;32:48-52.
30. Alderfer L, Wei A, Hanjaya-Putra D. Lymphatic tissue engineering and regeneration. J Biol Eng 2018;12:32.
31. Sestito LF, Thomas SN. Biomaterials for modulating lymphatic function in immunoengineering. ACS Pharmacol Transl Sci 2019;2:293-310.
32. Nguyen D, Zaitseva TS, Zhou A, et al. Lymphatic regeneration after implantation of aligned nanofibrillar collagen scaffolds: preliminary preclinical and clinical results. J Surg Oncol 2022;125:113-22.
33. Hadamitzky C, Zaitseva TS, Bazalova-Carter M, et al. Aligned nanofibrillar collagen scaffolds - Guiding lymphangiogenesis for treatment of acquired lymphedema. Biomaterials 2016;102:259-67.
35. Nguyen DH, Zhou A, Posternak V, Rochlin DH. Nanofibrillar collagen scaffold enhances edema reduction and formation of new lymphatic collectors after lymphedema surgery. Plast Reconstr Surg 2021;148:1382-93.
36. Deptula P, Zhou A, Posternak V, He H, Nguyen D. Multimodality approach to lymphedema surgery achieves and maintains normal limb volumes: a treatment algorithm to optimize outcomes. J Clin Med 2022;11:598.
37. Brazio PS, Nguyen DH. Combined liposuction and physiologic treatment achieves durable limb volume normalization in class II-III lymphedema: a treatment algorithm to optimize outcomes. Ann Plast Surg 2021;86:S384-9.
38. Boyages J, Kastanias K, Koelmeyer LA, et al. Liposuction for advanced lymphedema: a multidisciplinary approach for complete reduction of arm and leg swelling. Ann Surg Oncol 2015;22 Suppl 3:S1263-70.
39. Inchauste S, Zelones J, Rochlin D, Nguyen DH. Successful treatment of lymphedema in a vasculopath and neuropathic patient. J Surg Oncol 2020;121:182-6.
40. Hadamitzky C, Zaitzeva T, Paukshto M. Guided lymphangiogenesis for the treatment of lymphedema: preliminary clinical results. In 7th International Symposium in Cancer Metastasis through the Lymphovascular System: Biology & Treatment; 2017. Available from: https://www.jointechlabs.com/2021/01/11/guided-lymphangiogenesis-for-the-treatment-of-lymphedema-preliminary-clinical-results/ [Last accessed on 1 Nov 2022].
41. Dionyssiou D, Demiri E. A comprehensive treatment algorithm for patients requiring simultaneous breast and lymphedema reconstruction based on lymph node transfer. Ann Breast Surg 2021.
42. Schaverien MV, Butler CE. Hot topics in reconstructive surgery. Plast Reconstr Surg 2021;147:1245-7.
43. Jabbour S, Chang EI. Recent advancements in supermicrosurgical treatment of lymphedema. Plast Aesthet Res 2021;8:43.
44. Campbell KT, Silva EA. Biomaterial based strategies for engineering new lymphatic vasculature. Adv Healthc Mater 2020;9:e2000895.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Yesantharao PS, Nguyen DH. Nanofibrillar collagen scaffolds for lymphedema treatment: current applications and future directions. Plast Aesthet Res 2022;9:60. http://dx.doi.org/10.20517/2347-9264.2022.67
AMA Style
Yesantharao PS, Nguyen DH. Nanofibrillar collagen scaffolds for lymphedema treatment: current applications and future directions. Plastic and Aesthetic Research. 2022; 9: 60. http://dx.doi.org/10.20517/2347-9264.2022.67
Chicago/Turabian Style
Yesantharao, Pooja S., Dung H. Nguyen. 2022. "Nanofibrillar collagen scaffolds for lymphedema treatment: current applications and future directions" Plastic and Aesthetic Research. 9: 60. http://dx.doi.org/10.20517/2347-9264.2022.67
ACS Style
Yesantharao, PS.; Nguyen DH. Nanofibrillar collagen scaffolds for lymphedema treatment: current applications and future directions. Plast. Aesthet. Res. 2022, 9, 60. http://dx.doi.org/10.20517/2347-9264.2022.67
About This Article
Special Issue
Copyright
Data & Comments
Data
 Cite This Article 11 clicks
Cite This Article 11 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.