Anatomic variability of the vascularized composite osteomyocutaneous flap from the medial femoral condyle: an anatomical study
Abstract
Aim: The anatomical study and clinical application for the vascularized corticoperiosteal flap from the medial femoral condyle have been performed and described previously. Although prior studies have described the composite osteomyocutaneous flap from the medial femoral condyle, a detailed analysis of the vascularity of this region has not yet been fully evaluated.
Methods: This anatomical study described the variability of the arteries from the medial femoral condyle in 40 cadaveric specimens.
Results: The descending genicular artery (DGA) was found in 33 of 40 cases (82.5%). The superomedial genicular artery (SGA) was present in 10 cases (25%). All 33 cases (100%) of the DGA had articular branches to the periosteum of the medial femoral condyle. Muscular branches and saphenous branches of the DGA were present in 25 cases (62.5%) and 26 cases (70.3%), respectively.
Conclusion: The current study demonstrates that the size and length of the vessels to the medial femoral condyle are suffi cient for a vascularized bone flap. A careful preoperative vascular assessment is essential prior to use of the vascularized composite osteomyocutaneous flap from the medial femoral condyle, because of the considerable anatomical variations in different branches of the DGA.
Keywords
Introduction
The vascularized bone graft is the gold standard for reconstruction of bony defects, especially in case of chronic nonunion.[1] An anatomical studies and clinical applications for the use of a vascularized corticoperiosteal flap from the medial femoral condyle have been performed and described previously.[2,3] In 1991, Sakai and Doi and Sakai[4,5] initially reported the use of a thin, free vascularized corticoperiosteal graft for the treatment of persistent nonunion without significant bony defects in the upper limb. It has been demonstrated that the articular branch of the descending genicular artery (DGA) or the superomedial genicular artery (SGA) perfuses the medial femoral condyle. There are also two branches from the DGA which supply the muscle and skin at the level of the medial femoral condyle; the saphenous branch (SB) supplies the skin at the medial knee and proximal third of the leg, and the muscular branch (MB) normally runs into the vastusmedialis muscle.[4-7] This may allow the use of the DGA and its branches to form a composite osteomyocutaneous flap from the medial femoral condyle in the reconstruction of bony defects associated with avascular contracture of the soft tissue.
Although prior studies have described the composite osteomyocutaneous flap, the detail blood vessels in this region have not yet been fully elucidated. The aim of this study was to evaluate the anatomical variability of the vessels and their branches in the medial femoral condyle. Board of Hue Central Hospital approved the study.
Methods
Ten fresh and 10 formalin preserved adult cadavers were dissected in our study, consisting of 11 males and 9 females. Forty cadaveric specimens were harvested from both thighs. The osteomyocutaneous medial femoral condylar flap was elevated using the medial approach initially described by Sakai and Doi.[4,5,8] Cadavers were placed into the supine position and a 15-cm longitudinal incision was made medially along the posterior border of the vastusmedialis at the level of the distal femur, extending from the adductor hiatus proximally to the medial collateral ligament distally.[9-12] The fascia of the vastusmedialis was then incised, and the muscle was retracted superiorly while the adductor magnustendon was retracted inferiorly. The DGA was exposed on the floor of the muscle compartment proximally and on the surface of the medial femoral condyle distally. The SGA, a medial branch of the popliteal artery, was also studied. The anatomy of the DGA and SGA with their branches and their areas of distribution were dissected, measured, anddocumented. For the DGA, the length, location of origin, diameter, branches and terminations in the skin as well as in the periosteum overlying the medial femoral condylar region were determined. A dominant artery between the DGA and SGA was defined as a main artery supply to the medial femoral condyle.[7,13] The position of the artery was measured as the distance from the origin to the knee joint. The length of the artery was defined as the distance from its origin to the area of termination. The outer diameter (d) of the artery was calculated through the perimeter (P) of the peripheral arteries by the following formula: d = P/3.14.
The perimeter was calculated by flattening the artery at its origin and using a digital caliper (Anyi Instrument Co. Ltd, China) to measure its flat section, and then doubled. In the fresh cadavers, we also performed a dye injection at the origin of the articular and SBs of the DGA. This allowed visualization of the areas of the corticocancellous medial femoral condylar segment and skin paddle.[14,15] All measurements were recorded in millimeters, with an accuracy of 0.02 mm.
Results
The anatomical structures differed on the two sides of the thigh in the cadavers. The DGA origin from the superficial femoral artery (SFA) was found in 33 of 40 cases (82.5%). The DGA was absent in 7 cases. In 3 other cases, the DGA appeared together with the SGA. The SGA was present in 10 cases (25%). The DGA was dominant over the SGA in 33 of 40 cases (82.5%). In the remaining 7 cases (17.5%), the SGA was the major blood supply to the medial femoral condyle.
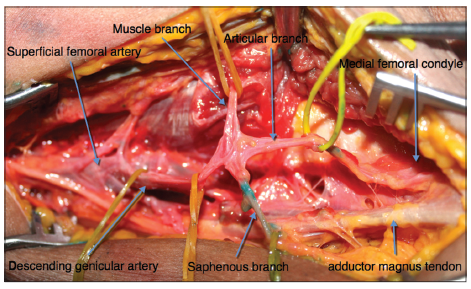
The DGA usually divided into branches; there were 11 (33.3%) cases of 2 branches, 21 cases (63.7%) of 3 branches and 1 (3%) case of 4 branches. The branches were the articular branches (AB), the SBs, and the MBs. The mean position of the DGA was 119.1 mm above the knee joint with a range of 96.2-148.8 mm (standard deviation [SD] 23.6 mm). The mean outer diameter of the DGA was 2.16 mm (range, 0.94-3.84 mm; SD 0.69 mm). From its origin to the onset of branching, there was a mean length of 11.7 mm (range, 0-40.33 mm; SD 8.61 mm) [Figure 1].
Figure 1. The vascular distribution of the descending genicular artery and its branches at the left femur in the fresh cadaver
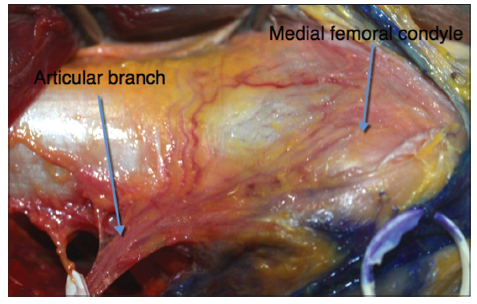
All 33 cases (100%) of the DGA sent AB to the periosteum of the medial femoral condyle. The AB further divided into smaller branches to the periosteum, with 1 branch in 19 cases, 2 branches in 13 cases, and 3 branches in 1 case. The mean location of its origin was 100.7 mm above the knee joint with a range from 70.3 to 129.4 mm (SD 13.4 mm). Its average length from the origin to the bone was 56.4 mm (range, 23.8-80.5 mm; SD 14.4 mm). The mean outer diameter was 1.5 mm (SD 0.4 mm). The mean area of the periosteum of the medial femoral condyle that the AB perfused was 37.8 mm × 25.7 mm [Figure 2].
Figure 2. Anatomy of the articular branch from the descending genicular artery for blood supply to the medial femoral condyle
In 39 (97.5%) cases the MB supplied blood to the distal aspect of the vastusmedialis muscle, and in 1 case the MB entered the gracilis muscle. In 25 cases (62.5%) the MB was a branch from the DGA, in 14 cases (36%) it came from the SFA, and in 1 case it branched off the AB. The mean length of the MB was 16.8 mm (SD 6.5 mm). The mean outer diameter was 1.6 mm (SD 0.9 mm).
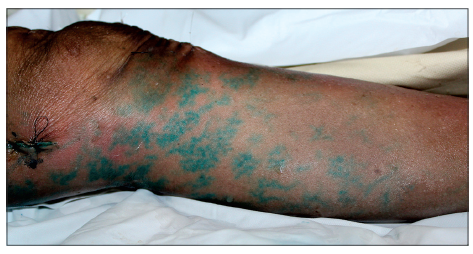
In 37 specimens (92.5%) the SB supplied the skin at the medial part of the knee and the proximal leg. In 3 specimens from the fresh cadavers, the SB ran to the gracilis muscle instead of toward the skin. The SB came off the DGA in 26 (70.3%) cases and the SFA in 11 (29.7%) cases. The mean location of the origin of the SB was 103 mm (SD 18.5 mm). Its mean outer diameter was 1.3 mm (SD 0.4 mm). Ten SB had 1 branch, and 27 SB had 2 branches to the skin at the medial part of the knee and the proximal part of the leg. In 13 specimens from the fresh cadavers, methylene blue was injected. A cutaneous angiosome distribution of the SB was noted on the medial aspect of the knee and proximal leg. The average perfusion area at the level of the skin was 244 mm × 115 mm [Figure 3].
Figure 3. Cutaneous angiosome distribution of the saphenous branch at the medial side of the knee and proximal leg after injected methylene blue in fresh cadavers
The superomedial genicular artery (SGA) existed in 10 (25%) specimens, and it was dominant over the DGA in 7 cases (17.5%). The mean outer diameter was 1.33 mm (SD 0.4 mm). The mean location of its origin was 88.5 mm (SD 17.8 mm) above knee joint. The mean length of the SGA to the periosteum was 37.5 mm (SD 16.9 mm).
Discussion
Either the DGA or SGA perfuse the medial femoral condyle. The current study evaluated the anatomical structures and variations of the DGA and SGA as well as their branches in adult cadavers. One half of cadavers were studied in fresh condition to facilitate the evaluation of the perfusion area of skin and bone.
Prior studies have shown that the outer diameter of the artery from fresh frozen cadavers was maintained. While the diameter of arteries from cadavers preserved in formalin retracts and loses its shape, the perimeter of the artery is maintained.[7] We calculated the outer diameter of the artery through its perimeter according to the following formula: P = 2R × 3.14 = d × 3.14 (R: radius = d/2). This measurement allowed us to determine the outer diameter in noninflated arteries.
Our study detected the DGA in 82.5% and the SGA in 25 of the 40 specimens. Yamamoto et al.[7] found the DGA in 89% and the SGA in 100% of the 19 specimens. Rahmanian-Schwarz et al.[1] harvested the DGA in 100% of the 21 specimens and Iorio et al.[16] also discovered the DGA in 100% of the 12 specimens. The difference between the studies is secondary to the number of specimens.
In the current study, the dominant vessels supplying the medial femoral condyle were the DGA in 82.5% of cases and the SGA in the DGA and 17.5% of cases. Van Dijck et al.[6] showed that in 70% of cases the DGA was dominant, while in 21% of cases the SGA was the dominant vessel. In 9% of cases the DGA and SGA supplied the medial femoral condyle equally. A comparison between the measurements of the DGA in the current study and other studies is made in Table 1.
The comparison between current and prior studies on anatomy of the DGA
Similar to previous studies, the current study demonstrated that the DGA generally divides into 3 branches (63.7% of cases) or 2 branches (33.3% of cases). In addition, the AB of the DGA or the SGA always nourishes the periosteum of the medial femoral condyle. These arteries have adequate diameter and length to supply the medial femoral condylar flap. In the absence of the DGA, the SGA has sufficient size, but the vascular pedicle is shorter, and SGA is used only for a pure bone flap.[8] The results of previous studies of Jones et al.[10] Yamamoto et al.[7], Van Dijck et al.[6] and De Smet[13] also made similar conclusions about the viability of this bone flap using the DGA or the SGA for treatment of small bony defects, especially in the treatment of nonunion fractures that require a good blood supply for bone grafting. In the specific study of Jones et al.[11], vascular pedicles of the vascularized medial femoral condylar flap for the treatment of scaphoid nonunion were the DGA in 10 cases and the SGA in 2 cases.[11]
In many cases of chronic nonunion, the soft tissue usually has a fibrous scar, infectious environment and avascular contracture. Extensive debridement of infected and devitalized tissue and bone back to bleeding tissue is required. Vascularized bone graft associated with a well-vascularized muscle or skin paddle is necessary in these cases. In the case of small bony defects (< 6 cm), the vascularized composite osteomyocutaneous flap from medial femoral condyle can fill the dead space of bone and soft tissue. It also minimizes the risk of deep tissue infection. By increasing the vascularity and the blood supply of the composite flap, limb salvage can be obtained with a single surgical procedure. Vascularized bone grafting can be combined with muscle tissue and a skin island, and thus can be used to solve complex problems in cases with bone and soft tissue defects.
The current study showed 100% of AB, 62.5% of MB, and 70.3% of SB branches come from the DGA. It allows the use of the medial femoral condylar bone flap, and this can be combined with muscle or skin in some cases. However, preoperative vascular assessment of this flap with an angiogram is very important due to the anatomical variation of the DGA as well as its muscular and SBs. This result differs from previous reports which studied fewer specimens; Iorio et al.[16] identified the SB in 11 of 12 specimens (92%). Rahmanian-Schwarz et al.[1] studied 21 specimens, and in 91.5%, the DGA split into three branches: AB, MB, and SB. Yamamoto et al.[7] showed that the SB was detected in 79% of their 19 specimens, branching off a common trunk with AB. Van Dijck et al.[6] found that the SB was present in 14 (41%) of the 27 cases.
The current study demonstrates that the size and length of the vessels supplying the medial femoral condyle are sufficient for a vascularized bone flap. This graft is very helpful in the treatment of chronic nonunion and small bone gap reconstruction. Although many studies have reported the viability of the vascularized composite osteomyocutaneous flap from the medial femoral condyle, a careful preoperative vascular assessment is essential secondary to the considerable anatomical variations in the different branches of the DGA. Further clinical studies will be required to clearly define the success of this composite osteomyocutaneous flap.
Acknowledgments
The authors would like to thank the Department of Anatomy, Ho Chi Minh University of Medicine and Pharmacy, Vietnam. We are grateful to Doctors LÊ Nghi Thanh Nhan, Paul Luu, Nguyen Van Phung, Tran Thiet Son and Peter Scougall for their excellent help and support.
Financial support and sponsorship
Nil.
Conficts of interest
None declared.
REFERENCES
1. Rahmanian-Schwarz A, Spetzler V, Amr A, Pfau M, Schaller HE, Hirt B. A composite osteomusculocutaneous free flap from the medial femoral condyle for reconstruction of complex defects. J Reconstr Microsurg 2011;27:251-60.
2. Bürger HK, Windhofer C, Gaggl AJ, Higgins JP. Vascularized medial femoral trochlea osteocartilaginous flap reconstruction of proximal pole scaphoid nonunions. J Hand Surg Am 2013;38:690-700.
3. Iorio ML, Masden DL, Higgins JP. The limits of medial femoral condyle corticoperiosteal flaps. J Hand Surg Am 2011;36:1592-6.
4. Doi K, Sakai K. Vascularized periosteal bone graft from the supracondylar region of the femur. Microsurgery 1994;15:305-15.
5. Sakai K, Doi K, Kawai S. Free vascularized thin corticoperiosteal graft. Plast Reconstr Surg 1991;87:290-8.
6. Van Dijck C, Mattelaer B, De Degreef I, De Smet L. Arterial anatomy of the free vascularised corticoperiosteal graft from the medial femoral condyle. Acta Orthop Belg 2011;77:502-5.
7. Yamamoto H, Jones DB Jr, Moran SL, Bishop AT, Shin AY. The arterial anatomy of the medial femoral condyle and its clinical implications. J Hand Surg Eur Vol 2010;35:569-74.
8. Doi K, Hattori Y. Vascularized bone graft from the supracondylar region of the femur. Microsurgery 2009;29:379-84.
9. Bakri K, Shin AY, Moran SL. The vascularized medial femoral corticoperiosteal flap for reconstruction of bony defects within the upper and lower extremities. Semin Plast Surg 2008;22:228-33.
10. Jones DB Jr, Bürger H, Bishop AT, Shin AY. Treatment of scaphoid waist nonunions with an avascular proximal pole and carpal collapse. A comparison of two vascularized bone grafts. J Bone Joint Surg Am 2008;90:2616-25.
11. Jones DB Jr, Moran SL, Bishop AT, Shin AY. Free-vascularized medial femoral condyle bone transfer in the treatment of scaphoid nonunions. Plast Reconstr Surg 2010;125:1176-84.
12. Kakar S, Duymaz A, Steinmann S, Shin AY, Moran SL. Vascularized medial femoral condyle corticoperiosteal flaps for the treatment of recalcitrant humeral nonunions. Microsurgery 2011;31:85-92.
13. De Smet L. Treatment of non-union of forearm bones with a free vascularised corticoperiosteal flap from the medial femoral condyle. Acta Orthop Belg 2009;75:611-5.
14. Del Pi-al F, García-Bernal FJ, Regalado J, Ayala H, Cagigal L, Studer A. Vascularised corticoperiosteal grafts from the medial femoral condyle for difficult non-unions of the upper limb. J Hand Surg Eur Vol 2007;32:135-42.
15. Rodríguez-Vegas JM, Delgado-Serrano PJ. Corticoperiosteal flap in the treatment of nonunions and small bone gaps: technical details and expanding possibilities. J Plast Reconstr Aesthet Surg 2011;64:515-27.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Thua TH, Bui DP, Pham DN, Lê VB, Mey AD, Boeckx W. Anatomic variability of the vascularized composite osteomyocutaneous flap from the medial femoral condyle: an anatomical study. Plast Aesthet Res 2014;1:85-8. http://dx.doi.org/10.4103/2347-9264.143544
AMA Style
Thua TH, Bui DP, Pham DN, Lê VB, Mey AD, Boeckx W. Anatomic variability of the vascularized composite osteomyocutaneous flap from the medial femoral condyle: an anatomical study. Plastic and Aesthetic Research. 2014; 1: 85-8. http://dx.doi.org/10.4103/2347-9264.143544
Chicago/Turabian Style
Thua, Trung-Hau Lê, Duc-Phu Bui, Dang-Nhat Pham, Vu-Bao Lê, Albert De Mey, Willy Boeckx. 2014. "Anatomic variability of the vascularized composite osteomyocutaneous flap from the medial femoral condyle: an anatomical study" Plastic and Aesthetic Research. 1: 85-8. http://dx.doi.org/10.4103/2347-9264.143544
ACS Style
Thua, T.H.; Bui D.P.; Pham D.N.; Lê V.B.; Mey AD.; Boeckx W. Anatomic variability of the vascularized composite osteomyocutaneous flap from the medial femoral condyle: an anatomical study. Plast. Aesthet. Res. 2014, 1, 85-8. http://dx.doi.org/10.4103/2347-9264.143544
About This Article
Copyright
Data & Comments
Data
 Cite This Article 1 clicks
Cite This Article 1 clicks











Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.