Comperative analysis of unilateral cleft lip closure using absorbable and nonabsorbable sutures: a randomised clinical study
Abstract
Aim: Patients with cleft lip usually undergo multiple procedures that require hospitalization resulting in emotional stress to their family members. Young patients often require sedation or general anesthesia (GA) for suture removal on a sensitive area to prevent disruption of the repair. In this study, we compared absorbable and nonabsorbable sutures for primary cleft lip repair.
Methods: Patients with cleft lip who presented to Smile Train Unit, Child Hospital and Research Institute, Nagpur, India, were randomly assigned to two groups and underwent surgical repair using either Vicryl Rapid suture (Group 1) or Prolene suture (Group 2). Patients were followed up at 1 month, 6 months, and 1 year. Photographs of the patients were obtained at these visits and rated using a validated 100-mm cosmesis visual analogue scale (VAS) by three people (social worker, surgeon, and patient’s mother). A VAS score of 15 mm or greater was considered as clinically important difference.
Results: A total of 60 patients were enrolled in this study, and they were equally divided into two groups. There was no difference in age, race, sex, wound length, number of sutures, and layered repair rates between the groups. The average age of the patient was 3 months. There was no significant difference in the rates of infection which was 6% in this study, wound dehiscence, and hypertrophic scar formation. No significant difference was found in cosmetic outcome in both the mean VAS score of 90.3 in Group 1 and 91.7 in Group 2.
Conclusion: Absorbable sutures are a viable alternative to nonabsorbable sutures in the repair of primary cleft lip repair. We prefer absorbable sutures because they do not require removal under GA or sedation.
Keywords
Introduction
Cleft lip and cleft palate are the most common craniofacial abnormalities seen worldwide. The prevalence of these anomalies ranges from 1:300-1200 live births for cleft lip and 1:2500 for cleft palate.[1] The history of surgical and aesthetic outcomes of cleft lip repair is fascinating.
The earliest attempts at cleft lip repair in China involved creating the raw edges and passing straight needles through each side of the wound.[1] The advent of modern suture materials and improved surgical techniques resulted in acceptable aesthetic outcome.[2] These congenital deformities have a significant psychological and socioeconomic effect on both the patient and their family. It often leads to disruption of psychosocial functioning and decreased quality of life.[3]
Current surgical repair involves anatomical dissection and geometric rearrangement of muscle, mucosa, and skin flaps to achieve an improved functional and cosmetic result.
The type of suture material used in surgery has been a long-standing debate among surgeons. Many surgeons prefer nonabsorbable suture material as it is easier to tie, unlikely to break prematurely, and induces minimal inflammatory response. Others feel that these issues are not important and prefer absorbable sutures because they do not have to be removed and thus, decreasing patient’s anxiety and discomfort.[4]
This study aims to compare the cosmetic outcomes and complications of primary cleft lip repaired with absorbable sutures versus nonabsorbable sutures. It also aims to identify a feasible surgical technique for Indian patients.
Methods
This study was conducted at the Smile Train Unit of Department of Cleft and Craniofacial Surgery at Child Hospital and Research Institute in Nagpur, India. The children's parents involved in this article agreed to publish their children’s facial pictures and signed the form. Patients with cleft lip who presented here from June 2010 to May 2012 were selected for this study with the following inclusion criteria:
1. Patients with unilateral primary cleft lip
2. Patients with 10 weeks age, 10 gm Hb %, and 10 pounds of weight
3. Patients physically fit to undergo general anesthesia (GA).
A total of 60 patients who met the criteria were included in this study, and they were divided into two groups randomly:
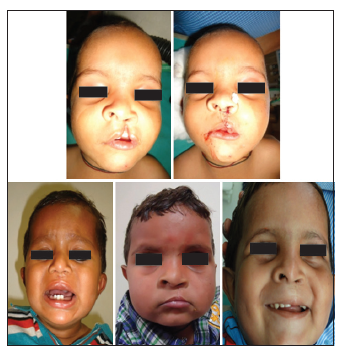
• Group 1: (n = 30) Cleft lip repair was performed using absorbable suture (Vicryl Rapid) [Figure 1].
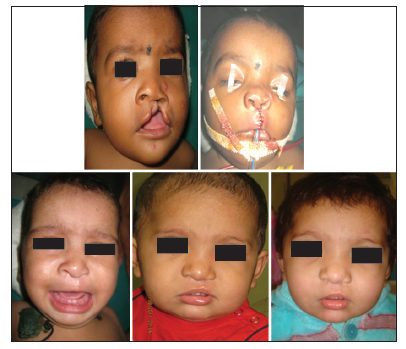
• Group 2: (n = 30) Cleft lip repair was performed using nonabsorbable suture (Prolene) [Figure 2].
Figure 1. Preoperative and postoperative photo at 1 month, 6 months, and 1 year follow-up for Group 1
Figure 2. Preoperative and postoperative photo at 1 month, 6 months, and 1 year follow-up for Group 2
All patients underwent routine blood tests, and informed consent was obtained from parents prior to surgery. The study was approved by the institution’s Ethical Committee. All patients underwent standard Millard’s rotational advancement technique by the same surgeon to repair the cleft lip. Patients were randomized by providing the surgeon with a sealed envelope that stated the type of suture to be used in the procedure before entering the operation theater.
All patients in Group 2 required GA or sedation for removal of sutures on 7th postoperative day.
Patients in both groups were evaluated for postoperative healing, infection rate, disruption of the wound, wound dehiscence, hypertrophic scar formation, and postoperative aesthetic outcome. Patients were followed and evaluated at 1 month, 6 months, and 1 year. Patient’s photographs were evaluated by three different people (social worker, surgeon and patient’s mother) using a validated 100 mm cosmesis visual analogue scale (VAS). In this study, a VAS score of 15 mm or greater was considered as a clinically significant difference.[5]
Descriptive statistical analysis was used to compare demographics and wound characteristics of the study groups. Differences between the groups were analyzed using variance analysis on rank data. VAS with a clinical difference of 15 mm or less was considered clinically significant.
Results
The average age of the patient was 3 months. There was no significant difference in the rates of infection which was 6% in this study, wound dehiscence, hypertrophic scar formation. There was no significant difference in the rates of infection, wound dehiscence, and hypertrophic scar formation. The postoperative wound infection was treated by oral amoxicillin in both groups [Table 1]. No significant difference was found in cosmetic outcome in both the groups with mean VAS of 90.3 in Group 1 and 91.7 in Group 2 [Tables 2-4].
Complications in both groups
| Complications | Number of patients | |
|---|---|---|
| Group 1 | Group 2 | |
| Infection | 2 | 2 |
| Wound dehiscence and disruption | 0 | 3 |
| Hypertrophic scar | 1 | 1 |
VAS scoring at 1 month
| VAS observer | Group 1 | Group 2 | P value |
|---|---|---|---|
| Observer 1 (blinded observer) | 87.1–90.6 (mean: 90.3) | 88.3–94.0 (mean: 91.7) | < 0.05 statistically no significant difference |
| Observer 2 (surgeon) | 89.1–93.6 (mean: 90.3) | 88.3–96.0 (mean: 91.7) | < 0.05 statistically no significant difference |
| Observer 3 (patients parent) | 78.4–90.1 (mean: 84.2) | 86.9–93.4 (mean: 90.1) | < 0.05 statistically no significant difference |
VAS scoring at 6 months
| VAS observer | Group 1 | Group 2 | P value |
|---|---|---|---|
| Observer 1 (blinded observer) | 88.1–94.6 (mean: 90.3) | 89.3–95.0 (mean: 91.7) | < 0.05 statistically no significant difference |
| Observer 2 (surgeon) | 88.1–94.6 (mean: 90.3) | 89.3–95.0 (mean: 91.7) | < 0.05 statistically no significant difference |
| Observer 3 (patient’s parent) | 76.4–92.1 (mean: 84.2) | 86.9–95.4 (mean: 90.1) | < 0.05 statistically no significant difference |
VAS scoring at 1 year
| VAS observer | Group 1 | Group 2 | P value |
|---|---|---|---|
| Observer 1 (blinded observer) | 88.1–94.6 (mean: 93.3) | 89.3–95.0 (mean: 92.7) | < 0.05 statistically no significant difference |
| Observer 2 (surgeon) | 88.1–94.6 (mean: 92.3) | 89.3–95.0 (mean: 93.7) | < 0.05 statistically no significant difference |
| Observer 3 (patients parent) | 76.4–92.1 (mean: 90.2) | 86.9–95.4 (mean: 93.1) | < 0.05 statistically no significant difference |
Discussion
Orofacial clefts are the most common head and neck congenital malformations. Cleft lip and cleft palate have significant psychological and socioeconomic effects on patient and affect their quality of life thus, requiring a multidisciplinary approach for management. The complex interplay between genetics and environmental factors plays a significant role in the formation this anomaly.[1]
The primary goals of surgical repair are to restore normal function for speech development and facial aesthetics.
Different techniques are employed based on surgeon’s expertise and patient’s anatomical variations. These patients undergo multiple surgical interventions at a very young age which poses a great challenge for the surgeons.
An understanding of both the physical properties of the material and the resulting tissue response to the material is important for choosing the suture material for the procedure. Sutures that are absorbable may initiate a prominent tissue response and result in suboptimal outcomes including a persistent scar, tenderness, and suture extrusion.[6]
To the best of our knowledge, there are very few studies reported in the literature that studied the cosmetic outcomes and complications after cleft lip using absorbable and nonabsorbable suture materials. Luck et al. compared the long-term cosmetic outcomes of absorbable versus nonabsorbable sutures for facial lacerations in children and concluded that fast-absorbing catgut suture is a viable alternative to nonabsorbable suture in the repair of facial lacerations in children.[7,8] Holger et al.[9] and Karounis et al.[10] compared the use of absorbable and nonabsorbable suture in traumatic pediatric lacerations and found no significant difference in the cosmetic outcome and complication rate.
Al-Abdullah et al.[11] performed a systematic review of randomized controlled trials that compared the cosmetic outcomes and complications of traumatic lacerations and found no statistically significant difference between absorbable and nonabsorbable sutures in short-term or long-term cosmetic score, scar hypertrophy, infection rate, wound dehiscence, and wound redness/swelling. This meta-analysis suggests a lack of large, methodologically sound study evaluating the effectiveness of absorbable versus nonabsorbable sutures.
Shinohara et al.[12] used monofilament nylon as nonabsorbable material and polyglyconate, polydioxanone as absorbable suture material and found no significant difference in the cosmetic appearance of the scars. These studies support the view that absorbable sutures are preferable to nonabsorbable sutures for primary cleft lip repair.[12,13] In addition, Collin et al.[14] published the disadvantages of using nonabsorbable sutures in cleft lip repair. These include a need for additional dressing, and return to the hospital for removal of the sutures under sedation or GA. All of these contribute to distress in the child and potential disruption of the repair.[14]
This study shows no significant difference between absorbable and nonabsorbable suture groups considering the cosmetic outcome in primary cleft lip repair. It has been shown that the VAS is a useful way to document subjective analysis of cosmetic outcome in this study.[5] As patients’ assessment of aesthetic outcome is subjective, the use of VAS in this study was appropriate.
A motivational factor to use an absorbable suture for cleft lip patients in this study was to avoid exposure to anesthesia for suture removal after 7 days. Furthermore, this study shows no clinically significant differences in cosmetic appearance between absorbable and nonabsorbable sutures at 1 month, 6 months, and 1 year. The results of this study are consistent with previously published reports.
This study demonstrates that there are no long-term differences in cosmetic outcome and complication rates between absorbable and nonabsorbable sutures in patients with primary unilateral cleft lip. All the patients enrolled in this study were operated by one surgeon using absorbable and nonabsorbable sutures and showed equal results. We recommend the use of absorbable suture for the closure of primary cleft lip as this technique saves one additional exposure of the child for the GA for suture removal.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
1. Sandberg DJ, Magee WP Jr, Denk MJ. Neonatal cleft lip and cleft palate repair. AORN J 2002;75:490-8.
2. Firth HV, Hurst JA. Clinical approach. In: Genetics. Oxford: Oxford Medical Press; 2006. pp. 74-7.
3. Marcusson A, Akerlind I, Paulin G. Quality of life in adults with repaired complete cleft lip and palate. Cleft Palate Craniofac J 2001;38:379-85.
4. Parell GJ, Becker GD. Comparison of absorbable with nonabsorbable sutures in closure of facial skin wounds. Arch Facial Plast Surg 2003;5:488-90.
5. Draaijers LJ, Tempelman FR, Botman YA, Tuinebreijer WE, Middelkoop E, Kreis RW, van Zuijlen PP. The patient and observer scar assessment scale: a reliable and feasible tool for scar evaluation. Plast Reconstr Surg 2004;113:1960-5.
6. Erel E, Pleasance PI, Ahmed O, Hart NB. Absorbable versus non-absorbable suture in carpal tunnel decompression. J Hand Surg Br 2001;26:157-8.
7. Luck RP, Flood R, Eyal D, Saludades J, Hayes C, Gaughan J. Cosmetic outcomes of absorbable versus nonabsorbable sutures in pediatric facial lacerations. Pediatr Emerg Care 2008;24:137-42.
8. Luck R, Tredway T, Gerard J, Eyal D, Krug L, Flood R. Comparison of cosmetic outcomes of absorbable versus nonabsorbable sutures in pediatric facial lacerations. Pediatr Emerg Care 2013;29:691-5.
9. Holger JS, Wandersee SC, Hale DB. Cosmetic outcomes of facial lacerations repaired with tissue-adhesive, absorbable, and nonabsorbable sutures. Am J Emerg Med 2004;22:254-7.
10. Karounis H, Gouin S, Eisman H, Chalut D, Pelletier H, Williams B. A randomized, controlled trial comparing long-term cosmetic outcomes of traumatic pediatric lacerations repaired with absorbable plain gut versus nonabsorbable nylon sutures. Acad Emerg Med 2004;11:730-5.
11. Al-Abdullah T, Plint AC, Fergusson D. Absorbable versus nonabsorbable sutures in the management of traumatic lacerations and surgical wounds: a meta-analysis. Pediatr Emerg Care 2007;23:339-44.
12. Shinohara H, Matsuo K, Kikuchi N. Absorbable and nonabsorbable buried sutures for primary cleft lip repair. Ann Plast Surg 1996;36:44-6.
13. Choudhary S, Cadier MA. Cleft lip repair: rub off the sutures, not the smile! Plast Reconstr Surg 2000;105:1566.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Datarkar AN, Rewanwar D, Rai A. Comperative analysis of unilateral cleft lip closure using absorbable and nonabsorbable sutures: a randomised clinical study. Plast Aesthet Res 2014;1:54-7. http://dx.doi.org/10.4103/2347-9264.139700
AMA Style
Datarkar AN, Rewanwar D, Rai A. Comperative analysis of unilateral cleft lip closure using absorbable and nonabsorbable sutures: a randomised clinical study. Plastic and Aesthetic Research. 2014; 1: 54-7. http://dx.doi.org/10.4103/2347-9264.139700
Chicago/Turabian Style
Datarkar, Abhay Nilkanth, Darshan Rewanwar, Anshul Rai. 2014. "Comperative analysis of unilateral cleft lip closure using absorbable and nonabsorbable sutures: a randomised clinical study" Plastic and Aesthetic Research. 1: 54-7. http://dx.doi.org/10.4103/2347-9264.139700
ACS Style
Datarkar, AN.; Rewanwar D.; Rai A. Comperative analysis of unilateral cleft lip closure using absorbable and nonabsorbable sutures: a randomised clinical study. Plast. Aesthet. Res. 2014, 1, 54-7. http://dx.doi.org/10.4103/2347-9264.139700
About This Article
Copyright
Data & Comments
Data
 Cite This Article 10 clicks
Cite This Article 10 clicks











Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.